Sarcoidosis and the eye
Sarcoidosis is a granulamatous multi-system disease with an unknown aetiology. It is characterised by its non-caseating granulomatous infiltration of epithelioid cells. The most common affects of the disease are bilateral hilar lymphadenopathy, pulmonary infiltration and skin and eye complications. Other organs involved include the liver, spleen, lymph nodes, salivary glands, heart, nervous system, joints, muscle and bones.
This disease is most common in African- Carribeans, Irish and Scandinavians. The incidence of the disease peaks at ages between 20-30 and also between 50-60 years. It is more common in women than in men. Around 80% of patients with Sarcoidosis are asymptomatic and go undiagnosed.
There has been some evidence that sarcoidosis may be triggered by several air-borne agents which can trigger the disease in susceptible individuals. Atypical mycobacteria have been suggested as a possible cause.
The eye is affected in up to 25-60% of patients with sarcoidosis.
Ocular manifestations:
Uvea
- Anterior uveitis – most common 60% of patients.
- This can be acute or chronic. Two thirds of patients will have chronic uveitis with large mutton-fat keratic precipitates, which are precipitates of inflammatory cells. Chronic uveitis may result in cataract, glaucoma and band keratopathy.
- One third will have acute uvetis which will usually be bilateral and symmetrical and also associated with bilateral hilar lymphadenopathy and erythema nodosum.
- Intermediate uveitis
- Chorioretinitis
- Koeppe (pupil margin) and Busacca (stromal) iris nodules.
- Choroidal granulomas
- Granulomas occur on the Lids, palpebral conjunctiva, optic nerve and orbit.
Lacrimal gland
- Granulomatous dacryoadenitis – This is a painless inflammation of the lacrimal gland.
- Infiltration of lacrimal glands à causing ‘dry-eye’ symptoms
Cornea and sclera
- Mutton fat keratic precipitates
- Keratoconjunctivitis sicca - reduced production of tears by the lacrimal glands. Often called 'Dry eye syndrome'.
- Calcific band keratopathy - Calcium deposition, in the appearance of a band, across the cornea.
- Scleritis - inflammation of the sclera
Lens
- Cataract
Retina/vitreous
- Vitritis - inflammation of the vitreous body
- Retinal neovascularisation – due to peripheral ischaemia or inflammation.
- Retinal vasculitis – focal perivascular exudates which appea as ‘candle wax drippings’, branch retinal vein occlusion can occur, focal venous sheathing, Cystoid macular oedema can cause visual loss.
- Epiretinal membranes – This is when scar tissue forms across the retina and distorts vision as the membrane contracts.
- Periplebitis - inflammation of the tissues around the veins.
Optic nerve
- Disc oedema – swelling could be due to raised intracranial pressure as a result of a cerebral granuloma. Papillitis can also occur in posterior uveitis when the optic nerve is involved.
- Neovasularistation
- Optic neuritis - inflammation of the optic nerve
- Optic atrophy - loss of optic nerve fibres
- Optic nerve granulomas
Neuro-opthalmic
- Pupil – Internal Opthalmoplegia, Argyll-Robertson pupil, Adie’s pupil
- Third, fourth and sixth cranial nerve palsies
Orbit
- Granulomas, Proptosis
Cystoid macular oedema (76%), cataract (49%), glaucoma (36%), retinal ischaemia (16%), and neovascularisations (11%) are frequent complications of posterior segment involvement in sarcoidosis.
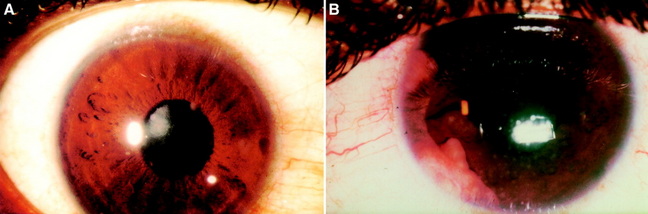
The images above show Anterior segment granulomas in two different patients with Sarcoidosis
A. Koeppe nodules are visible on the pupillary border
B. Large granulomas are seen in the anterior chamber of the eye in this patient.
A. Koeppe nodules are visible on the pupillary border
B. Large granulomas are seen in the anterior chamber of the eye in this patient.
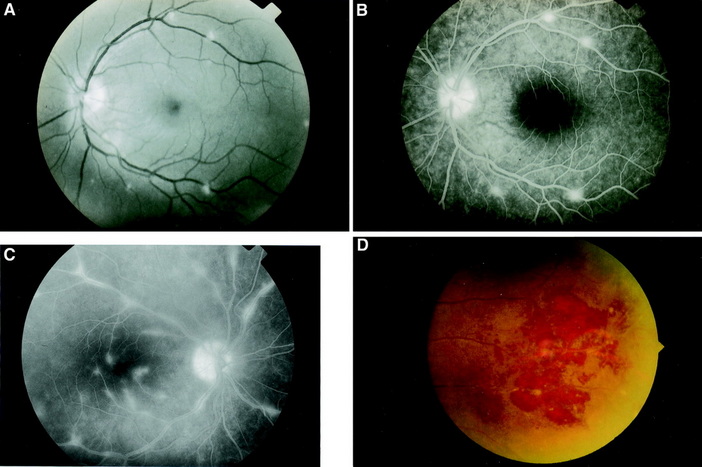
Retinal Vasculitis
A. Retinal Vasculitis showing focal perivascular inflammatory infiltrates
B. A Fluorescein Angiogram showing areas of focal perivenous leakage in the areas of vasculitis
C. Multiple perivascular leakages are seen in the Fluorescein angiogram
D. Peripheral retinal vessel sheathing surrounded with haemorrhages
A. Retinal Vasculitis showing focal perivascular inflammatory infiltrates
B. A Fluorescein Angiogram showing areas of focal perivenous leakage in the areas of vasculitis
C. Multiple perivascular leakages are seen in the Fluorescein angiogram
D. Peripheral retinal vessel sheathing surrounded with haemorrhages
All images above are used with permission from Dr Aniki Rothova.